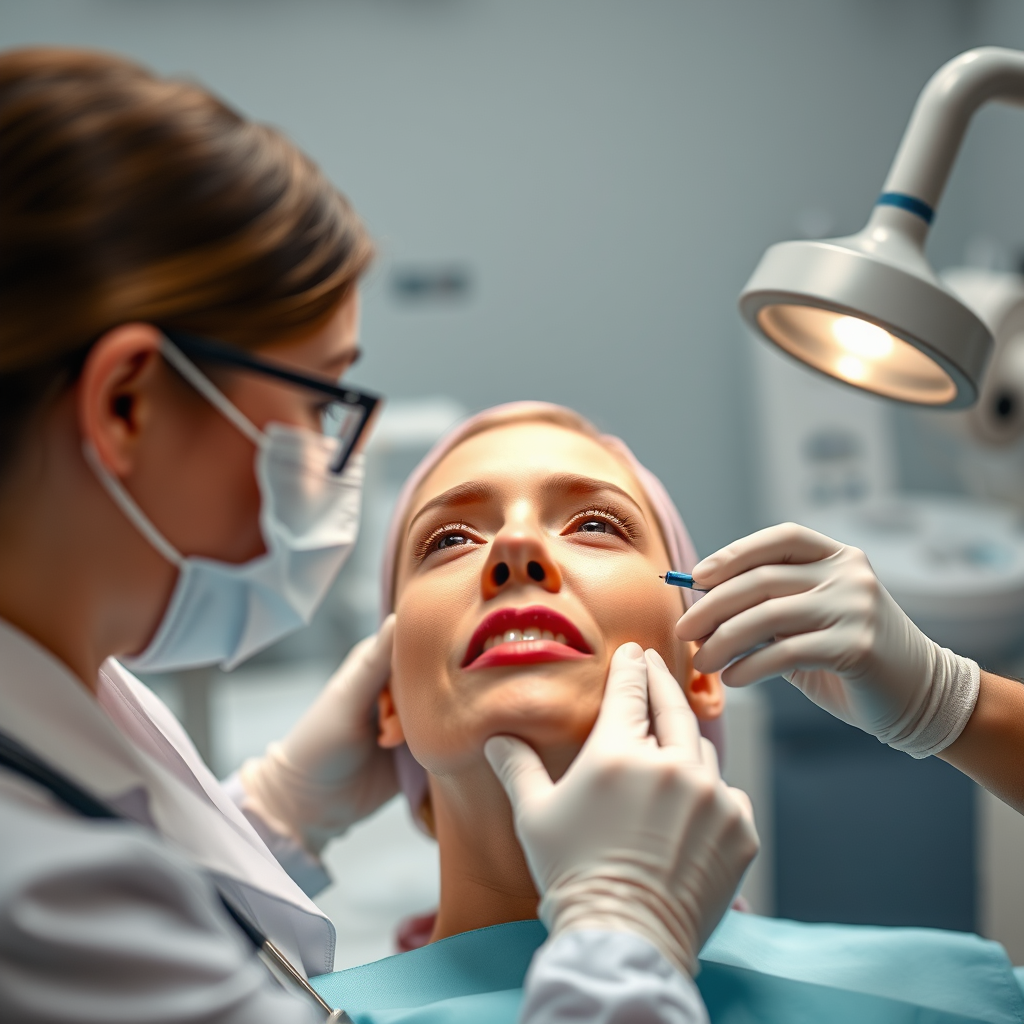
Insurance coverage for Botox as a treatment for temporomandibular joint (TMJ) disorders can vary widely, with some plans considering it a medical necessity while others do not. Understanding the nuances of your insurance policy and the specific criteria that may apply is essential for patients seeking relief from TMJ symptoms through Botox. In this article, we will explore the factors that influence insurance coverage for Botox, the conditions under which it may be deemed medically necessary, and the steps you can take to secure reimbursement.
Understanding TMJ Disorders
TMJ disorders encompass a range of conditions affecting the jaw joint and surrounding muscles, leading to discomfort and functional limitations. Common symptoms include jaw pain, headaches, clicking or popping sounds during jaw movement, and difficulty opening or closing the mouth. These disorders can arise from various causes, including jaw injury, teeth grinding (bruxism), stress, and arthritis.
Traditional treatments for TMJ disorders often include physical therapy, dental splints, and pain management strategies such as nonsteroidal anti-inflammatory drugs (NSAIDs). However, in recent years, Botox has emerged as a viable option for managing TMJ symptoms, particularly in cases where other treatments have proven ineffective.
The Role of Botox in TMJ Treatment
Botox, or botulinum toxin, is a neurotoxin that temporarily paralyzes muscle activity. When injected into the muscles surrounding the TMJ, Botox can effectively alleviate pain and reduce muscle tension, leading to significant relief for patients suffering from TMJ disorders. The mechanism behind this treatment involves blocking the nerve signals that lead to muscle contractions, thereby reducing spasms and discomfort.
The benefits of using Botox for TMJ treatment extend beyond pain relief. Many patients experience improved jaw function, reduced headaches associated with TMJ disorders, and an overall enhancement in quality of life. Furthermore, the effects of Botox typically last for three to six months, making it a manageable option for chronic TMJ pain.
Insurance Coverage Basics
When it comes to insurance coverage for medical treatments, the distinction between cosmetic and medically necessary procedures is crucial. Botox is often associated with cosmetic applications, such as wrinkle reduction; however, when used for TMJ treatment, it may be categorized differently. Insurers typically cover treatments deemed medically necessary, which involves a clinical assessment of the patient’s condition and the effectiveness of alternative treatments.
To qualify for insurance coverage, healthcare providers must demonstrate that the Botox treatment is essential for the patient’s well-being and is supported by clinical evidence. This often includes a thorough documentation process and adherence to specific guidelines established by the insurance company.
Factors Influencing Insurance Approval
Several factors can influence whether an insurance provider will approve coverage for Botox as a treatment for TMJ disorders. The most critical aspect is the documentation required to support the claim of medical necessity. This may entail comprehensive medical records, treatment history, and evidence that other conventional treatments have been attempted and were ineffective.
Your healthcare provider plays a significant role in the approval process. They must articulate the rationale for using Botox, emphasizing its potential benefits and outlining the patient’s specific needs. A well-documented case that includes diagnostic tests, treatment responses, and patient outcomes can greatly enhance the likelihood of receiving insurance approval.
Steps to Take for Coverage
To navigate the complexities of insurance coverage for Botox, start by contacting your insurance provider directly. Inquire about the specific policies related to Botox treatment for TMJ disorders and ask for clarification on what documentation is necessary for approval. Understanding your policy’s language is key, as some insurers may have specific criteria or exclusions related to this treatment.
If coverage is denied, do not lose hope. Many patients successfully appeal these decisions by providing additional information or clarifying the medical necessity of the treatment. Collect relevant documentation from your healthcare provider, including letters of medical necessity, treatment plans, and any supporting clinical studies that highlight the efficacy of Botox for TMJ. A well-structured appeal can make a significant difference in securing coverage.
Alternatives to Botox for TMJ
While Botox can be an effective treatment for TMJ pain, various alternatives are also available. Some common treatments include:
1. Physical Therapy: Targeted exercises can strengthen jaw muscles and improve flexibility, reducing pain and increasing function.
2. Dental Splints: Also known as occlusal splints, these custom-made devices help prevent teeth grinding and reduce strain on the jaw.
3. Medication: Over-the-counter pain relievers or prescription medications may be recommended for managing pain.
4. Stress Management Techniques: Since stress often exacerbates TMJ symptoms, practices such as mindfulness, yoga, and relaxation exercises can be beneficial.
Each alternative has its pros and cons. For example, physical therapy may require consistent commitment and time, while dental splints can take time to adjust to. Patients should consult their healthcare provider to determine the best course of action based on their specific circumstances.
Patient Experiences and Insights
Patient testimonials provide valuable insights into the journey of seeking Botox treatment for TMJ. Many individuals report significant relief from chronic pain and improved quality of life after receiving Botox injections. However, experiences with insurance coverage can vary widely.
Some patients have successfully navigated the insurance landscape with the help of their healthcare providers, while others have faced challenges. A common theme among those who encountered obstacles is the importance of persistence and thorough documentation. Engaging with healthcare providers to ensure a comprehensive understanding of the treatment’s medical necessity can greatly aid in the approval process.
In summary, understanding the intricacies of insurance coverage for Botox treatment in TMJ cases is vital for patients. While coverage may be available, it requires careful navigation of insurance policies, thorough documentation, and effective communication with healthcare providers. If you believe Botox may be the right option for your TMJ treatment, consult your healthcare provider to explore your options and take proactive steps to check your insurance coverage.
Frequently Asked Questions
Does insurance cover Botox injections for TMJ treatment?
Whether insurance covers Botox for TMJ (temporomandibular joint disorder) depends on your specific insurance plan and its policies regarding alternative treatments. Many insurance companies recognize Botox as a viable option for TMJ relief due to its ability to reduce muscle tension and pain. However, it’s essential to check with your insurer directly to understand your coverage options and any necessary pre-authorization requirements.
What conditions must be met for insurance to approve Botox for TMJ?
To have Botox for TMJ covered by insurance, you typically need to demonstrate that you have a diagnosed TMJ disorder and that previous conservative treatments, such as physical therapy or medications, have failed. Additionally, your healthcare provider may need to submit thorough documentation and possibly a treatment plan outlining the medical necessity of Botox as a treatment option.
How can I find out if my insurance covers Botox for TMJ?
The best way to find out if your insurance covers Botox for TMJ is to contact your insurance provider directly. You can call the customer service number on your insurance card and ask about coverage specifics for Botox treatments related to TMJ disorders. It’s also helpful to consult with your healthcare provider, as they may have experience working with insurance companies regarding similar claims.
Why is Botox used for treating TMJ, and how effective is it?
Botox is used for treating TMJ because it can effectively relax the muscles responsible for jaw clenching and grinding, which are common symptoms of TMJ disorder. Studies have shown that Botox can provide significant pain relief and reduce the frequency of headaches associated with TMJ. The effects typically last for three to six months, making it a valuable option for long-term management of TMJ symptoms.
What should I do if my insurance denies coverage for Botox for TMJ?
If your insurance denies coverage for Botox for TMJ, you can take several steps. First, review the denial letter for specific reasons and gather additional supporting evidence from your healthcare provider. You can then appeal the decision, providing documentation of your diagnosis, previous treatments tried, and a letter from your doctor explaining the medical necessity of Botox for your condition. Additionally, consider discussing alternative payment options or financing plans with your provider.
References
- https://www.ncbi.nlm.nih.gov/pmc/articles/PMC5837274/
- https://www.aaoms.org/docs/position_statements/botox_for_tmj_disorders.pdf
- https://www.americanheadachesociety.org/faq-botox-tmj-disorders/
- https://www.healthline.com/health/tmj-disorder/botox-for-tmj
- Hay fever – Diagnosis and treatment – Mayo Clinic